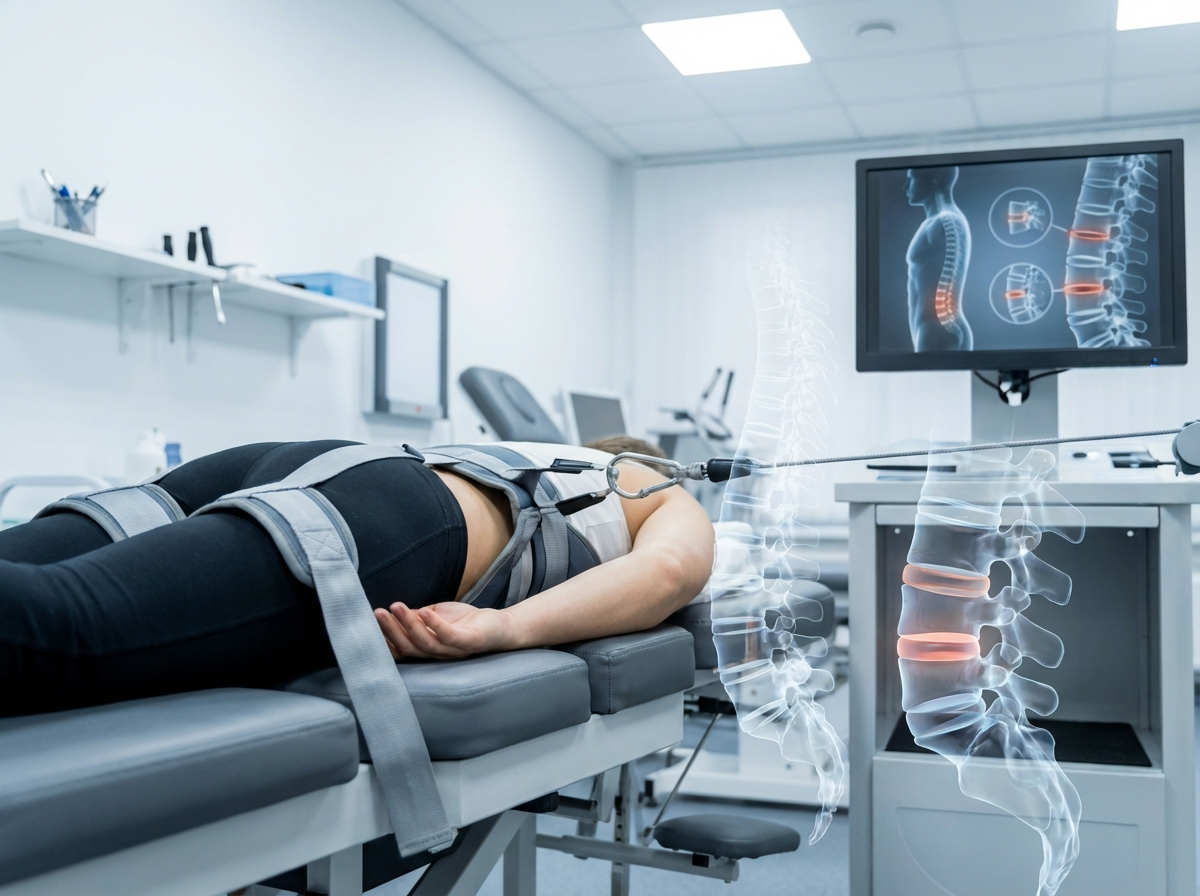
The Biomechanics of Spinal Decompression
As the spine experiences mechanical stress over time, the discs between vertebrae can compress and lose their cushioning function. This compression narrows the space between vertebrae and may cause nerves to become pinched, resulting in pain, numbness, or weakness.
Spinal decompression creates negative pressure within the disc through gentle, controlled stretching of the spine. You'll typically lie on a specialized table that moves in precise intervals, gradually separating vertebrae. This negative pressure accomplishes two critical functions: it pulls herniated disc material back toward its proper position and promotes the influx of oxygen, nutrients, and hydration into the disc.
The intermittent nature of the therapy—alternating between stretching and relaxation phases—helps overcome the body's natural muscle guarding response, allowing for more effective decompression than static stretching could achieve.
Understanding Intervertebral Disc Function
Intervertebral discs function as the spine's natural shock absorbers while enabling flexibility throughout your daily movements. Each disc consists of a tough outer layer (annulus fibrosus) surrounding a gel-like center (nucleus pulposus) that absorbs pressure and distributes force evenly across vertebrae.
These discs rely on proper hydration and nutrients, which they receive through a process called imbibition—the sponge-like absorption of fluids when pressure is relieved. Without this essential diffusion mechanism, discs become malnourished and degenerate prematurely.
As you age, your discs naturally lose water content and elasticity, becoming more vulnerable to bulging, herniation, and compression. This deterioration can restrict nerve pathways and trigger pain signals. Spinal decompression therapy aims to restore disc height and function by creating negative pressure that promotes rehydration and healing.
How Negative Pressure Creates Therapeutic Effects
Spinal decompression therapy works by creating negative intradiscal pressure that initiates a cascade of healing mechanisms within damaged discs. This negative pressure essentially creates a vacuum effect that helps pull herniated or bulging disc material back toward the center of the disc, reducing nerve compression.
When you undergo decompression therapy, you'll experience cycles of stretch and relaxation that pump nutrient-rich fluids and oxygen into the discs. These vital substances can't normally reach the discs' inner portions due to their avascular nature. The improved circulation promotes healing while simultaneously reducing inflammation.
The negative pressure also stimulates cellular repair mechanisms, encouraging the regeneration of damaged tissues and restoration of disc height. Your body's natural healing abilities are enhanced as pressure on pinched nerves decreases, often providing immediate pain relief while addressing the underlying structural problems.
Clinical Evidence and Research Findings
Research supporting spinal decompression therapy continues to grow, with multiple clinical studies demonstrating its effectiveness for treating various spinal conditions. A notable 2008 study in the Journal of Neuroimaging showed 71% of patients experienced significant pain reduction after treatment. You'll also find evidence in a 2014 systematic review that documented improved function in patients with lumbar disc herniation.
More recent research highlights how decompression therapy reduces intradiscal pressure, promoting healing of damaged discs. When comparing outcomes against traditional traction, studies reveal superior long-term results for non-surgical decompression, particularly for those with chronic back pain resistant to conventional treatments. While more rigorous trials are needed, the current evidence suggests you may experience substantial relief if you're suffering from disc-related disorders.
Comparing Surgical vs. Non-Surgical Decompression Methods
When considering treatment options for spinal pain, you'll face an important decision between surgical and non-surgical decompression approaches. Surgical methods like laminectomy, discectomy, and spinal fusion provide immediate pressure relief but carry risks of infection, nerve damage, and failed back surgery syndrome.
Non-surgical alternatives include mechanical traction tables, inversion therapy, and manual techniques. These options offer gradual improvement with minimal risk, though results may take longer to achieve. They're typically recommended before surgical intervention, especially for mild to moderate disc herniation, facet syndrome, or degenerative disc disease.
Your choice should depend on symptom severity, diagnostic imaging results, and response to conservative treatments. Many patients find lasting relief through non-surgical methods, while surgery remains valuable for severe cases with neurological compromise.
Ideal Candidates for Spinal Decompression Therapy
Not everyone benefits equally from spinal decompression therapy, which is why identifying suitable candidates remains crucial for treatment success. You're likely a good candidate if you suffer from herniated or bulging discs, degenerative disc disease, or posterior facet syndrome without advanced complications.
Ideal candidates typically exhibit persistent back pain that hasn't responded to conservative treatments like medication or physical therapy. You'll also need to be free from certain exclusionary factors including pregnancy, spinal fusion hardware, severe osteoporosis, spinal tumors, or fractures.
Your age matters too—patients between 25-65 generally respond best. If you're significantly overweight, have severe nerve damage, or suffer from spinal stenosis with structural abnormalities, you may need alternative treatments first.
Conditions That Respond Best to Decompression Treatment
Certain conditions consistently show remarkable improvement with spinal decompression therapy, making it a targeted intervention rather than a universal solution. You'll typically see the best results with herniated or bulging discs, where the therapy helps retract protruding disc material and reduces pressure on spinal nerves.
Degenerative disc disease also responds well, as the treatment promotes fluid exchange and nutrient flow to damaged discs. If you're suffering from posterior facet syndrome, sciatica, or spinal stenosis, decompression therapy can significantly reduce pain by creating negative pressure that alleviates nerve compression.
Patients with failed back surgery syndrome—persistent pain following spinal surgery—often find relief through this non-invasive alternative. The therapy works particularly well when your condition involves mechanical pressure on neural structures rather than inflammatory or systemic issues.
The Treatment Process: What to Expect During Sessions
Understanding the spinal decompression therapy process helps alleviate anxiety before your first appointment. During your initial session, you'll complete paperwork about your medical history and undergo a physical assessment. You'll then lie on a specialized table where the practitioner secures you with harnesses around your pelvis and trunk.
Each session lasts 20-45 minutes as the computerized system gradually stretches and relaxes your spine in controlled intervals. You'll feel a gentle pulling sensation but shouldn't experience pain. Many patients report the treatment is comfortable enough that they doze off.
Sessions typically occur 2-3 times weekly for 4-6 weeks. Your provider may complement decompression with heat therapy, electrical stimulation, or exercises to maximize results. Regular attendance is crucial for optimal outcomes.
Long-Term Outcomes and Maintenance Strategies
While successfully completing the treatment protocol marks a significant milestone, patients often wonder what happens after their final spinal decompression session. Most patients maintain their improvements for months or years following treatment, though individual results vary based on condition severity and lifestyle factors.
You'll need to protect your investment through regular maintenance strategies. These typically include specific strengthening exercises targeting your core and back muscles, proper ergonomics in daily activities, and periodic "booster" sessions every few months. Maintaining proper weight and staying hydrated also support long-term disc health.
Your provider will create a customized maintenance plan based on your specific condition and response to treatment. Following this plan diligently will maximize the durability of your results and minimize the chance of symptom recurrence.